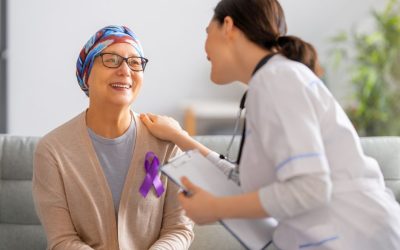
Cancer
According to the American Cancer Society, cancer affects one in 3 people in the US and is a major cause of mortality1. Cancer is a condition in which cells in our body grow and divide at a faster rate than normal. These cells can then form a mass, or complex tissue (called a tumor), can spread to other parts of our body and can lead to patient death. Tumor cell proliferation distances cells from the blood vessels which leads to lower levels of blood carrying oxygen in the tumor environment2. This low level of oxygen (hypoxia) activates certain molecules which regulate certain genes that tumor cells use to survive and resist treatment. Hypoxia is one of the ways tumors progress, resist, and metastasize, and is a common factor shared by all cancer types, including hematologic (blood cancers)2. Hyperbaric oxygen can be used to overcome hypoxia, inhibit and reduce cancer growth, and aid in the effectiveness of conventional therapies.
Extivita Therapies for Cancer:
Extivita Therapies for Cancer:

Hyperbaric Oxygen Therapy

Neurofeedback

Supplements

Nutritional IV Therapy

Pulsed Electromagnetic Field Therapy
Hyperbaric Oxygen Therapy for Cancer:

In addition, tumors under hypoxic conditions become more resistant to conventional therapies such as chemo and radiation. Given its deleterious effects in cancer, hypoxia is considered one of the best targets in treatment. Hyperbaric oxygen increases oxygen partial pressure which may suppress tumor growth, and when combined with chemo or radiation, can increase survival rate and minimize side effects(5).
Effects of HBOT on Cancer:

New Blood Vessel Formation
Increased Stem Cell Activity

Decreased Inflammation
IV Therapy for Cancer:
Hi Dose Vitamin C
Ascorbic acid (Vitamin C), when given in high concentration intravenously, has been clinically shown to elicit significant anti-cancer effects, while safe for healthy cells. Ascorbic acid at pharmacological levels, turns into hydrogen peroxide in the body and functions as a pro-oxidant, which selectively initiates cell death in cancer cells(6,7) . Hi dose intravenous Vitamin C (HDIVC) can be a non-toxic, low cost therapy to supplement HBOT and or standard of care in patients with cancer.
Myers Cocktail
The Myers cocktail infusion contains vitamins and minerals which can be used as supportive and protective therapy against chemo or radiation related side effects. Patients receiving standard of care (chemo/radiation) often complain of nausea, diarrhea, loss of appetite, fatigue, brain fog, anemia, mouth sores to name a few. Antioxidants in the Myers cocktail, when given apart from chemo/radiation, can significantly reduce side effects, improve quality of life, and possibly carry out standard of care therapy(8,9).
Neurofeedback for Cancer:
Neurofeedback (NF) has been tested for the positive effects it may have on those suffering from cancer-related impairments(10). Post-cancer cognitive impairment (PCCI), fatigue, peripheral neuropathy, sleep disturbance, and other psychological deficits are often a result of cancer treatments. Studies done on breast cancer survivors show that even after 5 years post-chemotherapy, participants who received NF therapy had significant improvements in all cognitive measures. Additionally, those patients who found improvement in cognitive impairment and fatigue also showed improvements in anxiety and depression in as little as 20 sessions(11). In those with Chemotherapy-induced peripheral neuropathy (CIPN), studies have shown that, after as little as 20 sessions, breast cancer survivors suffering from CIPN had a significantly decrease in pain, with no negative side effects recorded(12).

Pulsed Electromagnetic Field Therapy for Cancer:
Pulsed electromagnetic field therapy (PEMF) has been shown to exert selective killing effect on cancer cells, disrupt replication, suppress tumor blood vessel growth and induce cancer cells to self-destruct(13,15). PEMF is a therapy characterized by safe, low frequency electromagnetic fields (inducing microcurrents) applied to the entire body to target specific body tissues. Studies show PEMF presents several potential advantages including non-invasiveness, safety, lack of toxicity for non-cancerous cells, and the possibility of being combined with other available therapies(13). In vitro studies support pulsed electromagnetic field therapy’s ability to block formation of neoplasms and reduce growth of new blood vessels in cancer(13,14).
News & Research for Cancer:
Treating Cancer: How HBOT helps
Receiving a cancer diagnosis can be overwhelming, especially when it comes to finding the most effective treatment for your diagnosis. That’s why our Nurse Practitioner, Elena Schertz and the team at Extivita-RTP provide personalized attention and compassionate...
Oxygen therapy can kill cancer cells available in Mexico
Alternative treatments for cancer do exist. Consider hyperbaric oxygen therapy. Oxygen therapy has different treatment methods that are designed to stifle tumors and cancerous cells using oxygen. There are different ways of applying these treatments that range from...
Mom Can Play With Her Daughters Again After Breast Cancer
Specialized Expertise by Holmdel's Dr. Asaad H. Samra, M.D., Hackensack Meridian Bayshore Medical Center, Gives Local Mom Her Life Back.Photo Credit: HMHUBy HACKENSACK MERIDIAN HEALTH U Published October 2, 2022 at 10:08 AM HOLMDEL, NJ: Six months after a double...
References
- https://www.cancer.org/treatment/understanding-your-diagnosis/what-is-cancer.html
- Hanahan, Douglas, and Robert A Weinberg. “Hallmarks of cancer: the next generation.” Cell vol. 144,5 (2011): 646-74. doi:10.1016/j.cell.2011.02.013
- J. Cui, X. Mao, V. Olman, P. J. Hastings, Y. Xu. Hypoxia and miscoupling between reduced energy efficiency and signaling to cell proliferation drive cancer to grow increasingly faster. Journal of Molecular Cell Biology, 2012; DOI: 10.1093/jmcb/mjs017
- Moen, Ingrid, and Linda E B Stuhr. “Hyperbaric oxygen therapy and cancer–a review.” Targeted oncology vol. 7,4 (2012): 233-42. doi:10.1007/s11523-012-0233-x
- Chen, SY., Tsuneyama, K., Yen, MH. et al. Hyperbaric oxygen suppressed tumor progression through the improvement of tumor hypoxia and induction of tumor apoptosis in A549-cell-transferred lung cancer. Sci Rep 11, 12033 (2021). https://doi.org/10.1038/s41598-021-91454-2
- Vollbracht, Claudia et al. “Intravenous vitamin C administration improves quality of life in breast cancer patients during chemo-/radiotherapy and aftercare: results of a retrospective, multicentre, epidemiological cohort study in Germany.” In vivo (Athens, Greece) vol. 25,6 (2011): 983-90.
- Markowska, Anna et al. “Role of Vitamin C in Selected Malignant Neoplasms in Women.” Nutrients vol. 14,4 882. 19 Feb. 2022, doi:10.3390/nu14040882
- Böttger, Franziska et al. “High-dose intravenous vitamin C, a promising multi-targeting agent in the treatment of cancer.” Journal of experimental & clinical cancer research : CR vol. 40,1 343. 30 Oct. 2021, doi:10.1186/s13046-021-02134-y
- Markowska, Anna et al. “Role of Vitamin C in Selected Malignant Neoplasms in Women.” Nutrients vol. 14,4 882. 19 Feb. 2022, doi:10.3390/nu14040882
- Hetkamp, Madeleine, et al. “A Systematic Review of the Effect of Neurofeedback in Cancer Patients.” Integrative Cancer Therapies, Jan. 2019, doi:10.1177/1534735419832361
- Alvarez, Jean, et al. “The Effect of EEG Biofeedback on Reducing Postcancer Cognitive Impairment.” Integrative Cancer Therapies, Nov. 2013, pp. 475–487, doi:10.1177/1534735413477192.
- Prinsloo, Sarah, et al. “Randomized controlled trial of neurofeedback on chemotherapy-induced peripheral neuropathy: A pilot study.” Cancer vol. 123,11 (2017): 1989-1997. doi:10.1002/cncr.30649
- Vadalà, Maria, et al. “Mechanisms and Therapeutic Effectiveness of Pulsed Electromagnetic Field Therapy in Oncology.” Cancer Medicine, John Wiley and Sons Inc., Nov. 2016,
- Crocetti S., Beyer, C., Schade, G., Egli M., Fröhlich J., Franco-Obregón A. “Low Intensity and Frequency Pulsed Electromagnetic Fields Selectively Impair Breast Cancer Cell Viability.” PloS One, U.S. National Library of Medicine, 2013,
- Zimmerman, J. W., M. J. Pennison, I. Brezovich, N. Yi, C. T. Yang, R. Ramaker, et al. 2012. Cancer cell proliferation is inhibited by specific modulation frequencies. Br. J. Cancer 106:307–313.