Treating Calciphylaxis with HBOT
In the realm of medical breakthroughs, there are few treatments as remarkable as hyperbaric oxygen therapy (HBOT). With its ability to harness the healing potential of oxygen, HBOT has emerged as a groundbreaking approach for numerous medical conditions. Among its remarkable applications, HBOT has recently gained attention for its potential to heal calciphylaxis, a rare and devastating condition characterized by painful skin ulcers and tissue necrosis.
Calciphylaxis, also known as calcific uremic arteriolopathy, primarily affects individuals with underlying chronic kidney disease. It is a multifactorial disease that arises when calcium and phosphate deposits accumulate within the walls of small blood vessels, resulting in restricted blood flow. As a consequence, the affected skin and underlying tissues are deprived of oxygen and vital nutrients, leading to the formation of non-healing wounds and, in severe cases, even amputation and death.
Healing Calciphylaxis Using HBOT
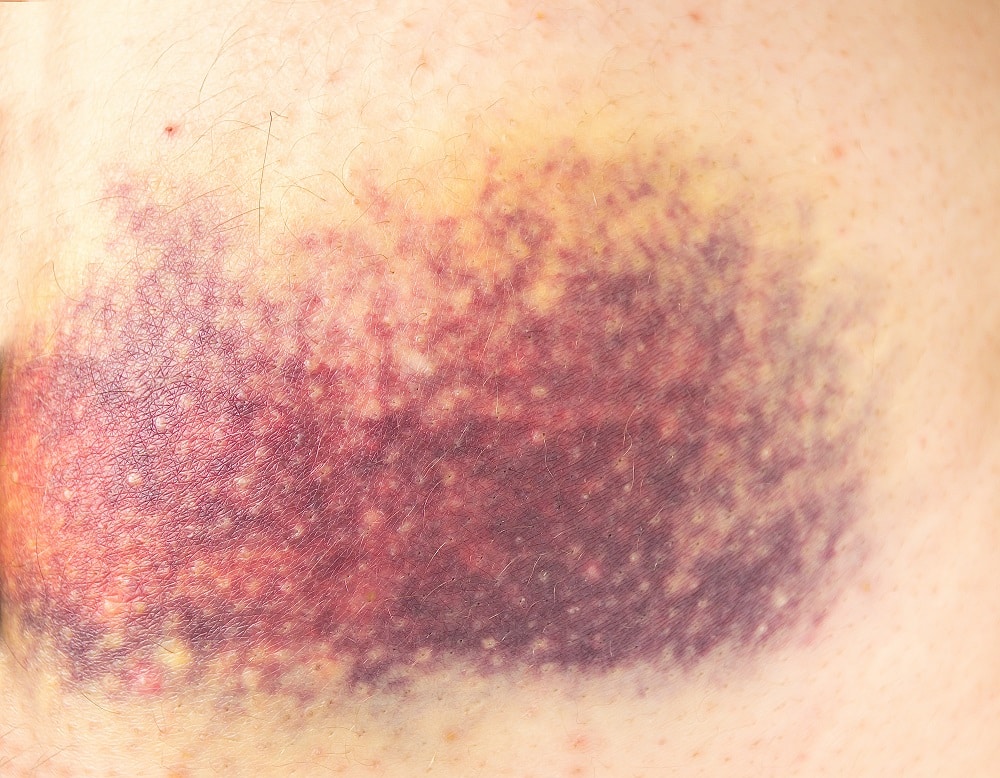
Traditionally, the treatment options for calciphylaxis have been limited and often ineffective. However, the discovery of HBOT’s potential in healing calciphylaxis has opened up new avenues of hope for patients and medical professionals alike. HBOT involves the administration of 100% pure oxygen in a pressurized chamber, allowing the patient to breathe in higher oxygen levels compared to what is available in normal atmospheric conditions. This increased oxygen concentration dissolves into the bloodstream, reaching even the most compromised areas of the body.
The healing mechanism of HBOT in calciphylaxis is multifaceted. By supplying a surplus of oxygen, HBOT helps to bypass the restricted blood flow and directly nourish the oxygen-starved tissues. Furthermore, the increased oxygen levels stimulate the growth of new blood vessels, a process known as angiogenesis, which aids in improving blood circulation and tissue repair. HBOT also has anti-inflammatory effects, reducing inflammation and pain associated with calciphylaxis.
Research into the effectiveness of HBOT for calciphylaxis is still ongoing, but early studies and clinical observations have yielded promising results. Many patients have experienced substantial improvements in wound healing, reduction in pain, and even complete resolution of ulcers following HBOT sessions. While each case is unique, the growing body of evidence suggests that HBOT can significantly enhance the quality of life for those afflicted by calciphylaxis.
It is important to note that HBOT is a complementary therapy that works in conjunction with other treatments for calciphylaxis. A multidisciplinary approach involving dermatologists, nephrologists, and wound care specialists is typically employed to provide holistic care to patients. This collaborative effort aims to address the underlying causes of calciphylaxis, manage pain, promote wound healing, and prevent further complications.
Research Findings
At a single center, 25 Norwegian patients with calciphylaxis received hyperbaric oxygen as part of multidisciplinary care during 2012-2022. While in a hyperbaric chamber, patients receive 100% oxygen delivered at above-normal air pressure. Normal air is 21% oxygen. Patients received a median 45 hyperbaric oxygen treatments in addition to conventional care, including sodium thiosulfate, dialysis if needed for calcium-phosphate homeostasis, vitamin K2, withdrawal of warfarin, iron, and vitamin D, limited use of systemic steroids, and weight and nutritional interventions. A recent meta-analysis concluded that intravenous sodium thiosulfate treatment provides no benefit in these patients.
Within 1 year, 7 patients died of cardiovascular disease, infection, or cancer. Of the 18 survivors, 15 (83%) had experienced wound healing.
Calciphylaxis is known to be fatal in up to half of patients, the investigators noted. Treatment options are limited. Hyperbaric oxygen may be a helpful adjuvant therapy.
“Hyperbaric oxygen therapy may improve wound healing by increasing tissue oxygenation,” Espen Nordheim, MD, PhD, of Oslo University Hospital in Norway, and colleagues explained. “Our impression is that [hyperbaric oxygen therapy] is well-tolerated and associated with less wound-associated pain.”
The survival rate in this study was higher than reported in other case series. Future research is needed to determine whether hyperbaric oxygen therapy can prolong life.
Cited by: Renal & Urology News
