Treating Veterans with TBI & PTSD
Between 2000 and 2020, more than 430,000 US Service Members have experienced their first lifetime Traumatic Brain Injury (TBI), not including service members who incur subsequent TBI’s(1). TBI’s are classified as mild, moderate, severe, or penetrating. They can occur from a sudden blow or jolt to the head from an impact, blast exposure, and even whiplash. Studies suggest that service members and veterans who have sustained a TBI may still have ongoing symptoms of post-concussive syndrome that go untreated. TBI of any severity can cause symptoms across multiple functional domains, including physical, cognitive, and psychological.
In addition, among veterans with positive TBI screens, 80% indicate comorbid psychiatric diagnosis and up to half meet criteria for Post-Traumatic Stress Disorder (PTSD)(2). From the Vietnam war to Operation Enduring Freedom, Veterans suffering from PTSD has increased from 15% to 20%. PTSD is a complex psychiatric condition that develops in certain individuals after experiencing a major traumatic event(14). Behavioral symptoms of PTSD include re-experiencing the trauma, avoidance behavior, mood alternation, and hyperarousal(15).
The negative impact that such symptoms and risks can make on one’s quality of life makes it clear that veterans with PTSD and TBI’s require safe, effective treatment options. Unfortunately, less than half of patients receiving traditional psychosocial treatments gain clinically meaningful improvements, and many continue to have residual symptoms(22-23). Thankfully, there is compelling evidence to suggest that Hyperbaric Oxygen Therapy (HBOT) may significantly reduce the negative symptoms experienced by TBI patients and PTSD patients, even years after the incident.
Extivita Therapies for Veterans Suffering from TBI or PTSD:
Request More Information:
Sponsor HBOT for Veterans
At Extivita, we’re dedicated to making the treatment of TBIs and PTSD affordable and available to those who have served in the United States Military. In 2022, the State of North Carolina has generously set aside $150,000 to help US Veterans get Hyperbaric Oxygen Therapy.
With so many veterans needing this therapy, those funds will quickly dissipate. They served our country, help us serve them by donating a dive, multiple dives, or by sponsoring a veteran.
Corporate giving opportunities are available as well. The Steel Network, Inc. a veteran owned light steel framing manufacturer in Durham, North Carolina currently matches all HBOT donations for US Military Veterans and First Responders at Extivita.
What is Hyperbaric Oxygen Therapy?
HBOT involves sitting in a hyperbaric chamber while breathing 100% medical grade oxygen through a mask or hood. The hyperbaric chamber gradually pressurizes to between 1.5 and 2.5 times the normal atmospheric pressure (referred to as 1.5 ATA and 2.5 ATA). This is equivalent to diving between 16 feet (1.5 ATA) and 50 feet (2.5 ATA) below water.
The majority of HBOT treatments at Extivita are at 2.0 ATA, which is equivalent to 33 feet below surface level. Because oxygen is considered a drug by the FDA, patients must obtain a prescription from a licensed healthcare professional for these therapeutic treatments. The specific pressure is also included in the prescription. Our in-clinic provider can write HBOT prescriptions following your in-person consultation.
How does Hyperbaric Oxygen Therapy affect TBI & PTSD?
HBOT has been shown to improve cognitive function and quality of life in patients who experienced a mild TBI(4). Additionally, HBOT results in improved cognitive function (in multiple categories) in the case of moderate and severe TBI. These improvements were correlated with increased activity in the brain regions associated with each cognitive impairment(4).
HBOT also can have positive behavioral and neurochemical effects in patients with PTSD by regulating the immune system. Emerging evidence suggests that patients with PTSD have biological alterations, such as a dysregulated immune system, which results in oxidative stress and inflammation(24,26). In fact, a 2015 meta-analysis of 20 studies found that PTSD is associated with elevated levels of proinflammatory markers in the blood plasma and serum(25,26).
The consequences of oxidative stress and inflammation include accelerated cellular aging as well as increased risk of neurological, cardiovascular, and respiratory diseases. Taken together, the effects of increased disease risk increase the physical and emotional burden of those with PTSD(26). Thankfully, HBOT has been shown to inhibit many of the same proinflammatory cytokines (chemical messengers) that are elevated in PTSD, while also increasing anti-inflammatory/antioxidant gene expression(27). By doing so, HBOT may improve some of the chemical imbalances that can cause serious damage to those with PTSD.
Effects of HBOT on the Body:

New Blood Vessel Formation
Increased Stem Cell Activity

Decreased Inflammation
Research suggests that increased tissue oxygenation, improved cellular metabolism and mitochondrial function, and improved inflammatory response, to name a few, are responsible for improving the following cognitive impairments(5):
- Improved Memory (most improvement)
- Reduced Attention Problems (high improvement)
- Improved Executive Function
- Increased Information Processing Speed
- Improved Motor Skills
Frequently Asked Questions About Hyperbaric Oxygen Therapy
How do I get started with HBOT (new patients)?
Before you come into the clinic, you will need to register as a patient in our patient portal. Here you will enter your medical history and primary reason/s for starting HBOT. After this, you will be able to schedule a consultation with Elena Schertz, FNP. You will be all set to begin treatment following your consultation!
How is HBOT administered?
What type of HBOT chambers do we use?
What can I do while in the HBOT chamber?
Will I be by myself during my HBOT session?
There will be a trained Extivita supervisor with you in all HBOT sessions. While you may be the only patient in the chamber on some days, most sessions will have other patients in the chamber as well. For additional information on how we are keeping our patients safe during COVID-19, click here.
How long does an HBOT session last?
How many HBOT sessions are needed to improve PTSD and TBI Symptoms?
This depends on the condition that you are receiving treatment for, as well as how your body responds to HBOT. The antioxidant and anti-inflammatory effects of HBOT can typically be felt within the first few sessions. Benefits for acute injuries and soft-tissue damage can typically be seen 5-10 sessions in, while chronic injuries typically require 10-20 sessions. Many conditions require 20-40 HBOT sessions for full healing effects such as stem cell increase.
For TBI and PTSD patients, an initial HBOT regimen is typically 40 sessions. Symptom improvement is often experienced by patients between 10 and 20 sessions.
Are there any side-effects to HBOT?
HBOT is generally considered one of the safest therapies in use today. Any serious side effects can be prevented by pre-HBOT screening that all patients receive during their consultation. One side effect that is some people experience is mild ear pain while the chamber pressurizes. However, this can be reduced through proper sinus clearing and it typically goes away as you receive more treatments.

Neurofeedback for Veterans with PTSD & TBI:
Neurofeedback has been shown to improve many of the cognitive issues that veterans with traumatic brain injuries (TBIs) experience post-injury(6, 7). After a TBI, the brain must form new neural pathways to account for any brain tissue damaged by the TBI. These new connections play a vital role in restoring healthy brain function, and neurofeedback has been shown to help establish and help strengthen such connections(6). Most studies that use neurofeedback to help TBIs train to increase theta and alpha brainwaves in the occipital lobe (towards the back of the head). This has been shown to reduce stress (which has a negative physiological and emotional effect in TBIs), increase relaxation, and improve cognitive measures such as memory and processing speed (6, 7, 8, 9).
Additionally, Neurofeedback therapy has strong potential as an effective, non-invasive therapy for those with PTSD. Individuals with PTSD are believed to have a degree of dysfunction in two important neural networks: the salience network (SN) and the default mode network (DMN) (23-24). Normalizing these networks through neurofeedback has been shown to significantly improve symptoms of PTSD (21-29). To normalize these networks, neurofeedback protocols for PTSD typically focus on reducing theta and high-beta while increasing low-beta activity(27, 30) or decreasing alpha activity(12,13). Both protocols have shown to significantly improve symptoms of PTSD and improve emotional regulation after 20-40 neurofeedback sessions.
IV Therapy for Veterans with PTSD & TBI:
The combination of the Myer’s cocktail and glutathione IV’s can improve cognitive and motor function following traumatic events and brain injury. A principal issue post-TBI is the degree neuroinflammation, which is directly correlated to the severity of the short-term and long-term consequences of TBI. In TBI patients, the mitochondria in brain cells become damaged, activating immune cells (glia, microglia, and astrocytes). These immune cells release inflammatory cytokines which recruit even more inflammatory cells to the area. This results in brain cell swelling, death, decreased energy production, all of which lead to impaired cognitive and motor function(10).
The Myer’s cocktail can help minimize further cells damage and improve brain health and function for those suffering PTSD, or after a TBI(11, 12). One of the primary issues in PTSD is the repeated pattern of re-experiencing the traumatic event, which results in chronic activation of the body’s stress response(36). Additionally, the sleep disruption, hypervigilance, anger, anxiety and dysphoria that most people with PTSD experience also activate the stress response. The net effect of this is hyperactivation of the stress network which results in oxidative damage(36). The Myer’s Cocktail IV contains Vitamin C and other nutrients which have been shown to counteract increases in stress hormones(37-38).
Glutathione, the master antioxidant, has been used to reduce oxidative stress and enhance cellular detoxification and can be part of a multi-modal therapy in correcting the metabolic crisis in TBI. Research also shows that levels of Glutathione are imbalanced in patients with PTSD(39). Our Glutathione IV can increase Glutathione levels in the body to reduce oxidative stress and enhance cellular detoxification.
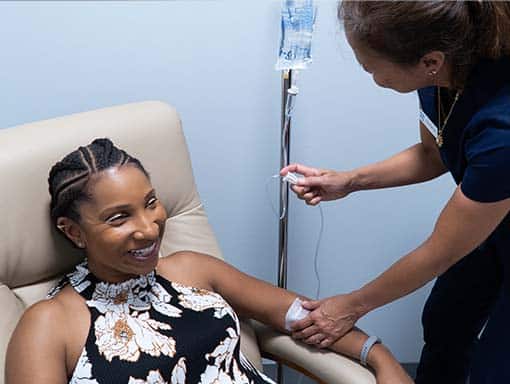
PEMF Therapy for Veterans with PTSD & TBI:
Pulsed-electromagnetic field therapy (PEMF) results in improved microcirculation, as well as increased oxygen and nutrient delivery to much needed areas of the body. Micro vessels play a significant role in overall course of vascular diseases. Dysfunction to this system has been linked to a multitude of illnesses. The PEMF device has been shown to optimize the microcirculatory system for veterans suffering from TBIs and/or PTSD, increasing perfusion to tissues and organs. When used in conjunction with HBOT, oxygen rich blood can be delivered to these areas, where healing can begin(13).
Additionally, PEMF has been shown to reduce levels of inflammation, which is a primary culprit in PTSD pathology(40, 21). The BEMER also has an accessory called the B-pad which can be utilized to target specific regions for better pain management. In cases of neurological concerns like PTSD, we can even position the B-pad over the individual’s head to maximize PEMF’s therapeutic benefits.
News & Research for Veterans with PTSD & TBI:
Extivita Expands to Jacksonville, NC—Bringing Life-Changing Therapies to the Coast
Jacksonville, NC – Extivita, North Carolina’s leading center for Hyperbaric Oxygen Therapy (HBOT) and integrative wellness services, is excited to announce the opening of its newest clinic in Jacksonville, NC—a region defined by military service, resilience, and a...
Redefining our Approach to Reduce Veteran Suicide – An ordinary man’s extraordinary quest using Hyperbaric Oxygen Therapy
Written by: Karee White The escalating rate of Veteran suicides, reaching 6392 in 2021, an increase of 114 from the previous year (U.S. Department of Veterans Affairs, 2023), has spurred numerous organizations to combat this crisis. Despite dedicated efforts and a...
HBOT: A Lifeline for Veterans and the Promise of Extivita’s RDU Clinic
Hyperbaric Oxygen Therapy (HBOT) has been gaining attention in the medical community for its transformative impact on numerous health conditions. A recent article in the Durango Herald highlights the story of a Bayfield veteran who believes that HBOT saved his life,...
References:
- Report to Congress, Study and Report on Traumatic Brain Injury Mitigation Efforts Final Report, July 2021. US Department of Defense. https://www.cdc.gov/traumaticbraininjury/pdf/Report_to_Congress_on_Traumatic_Brain_Injury_2013-a.pdf
- Mac Donald CL, Johnson AM, Wierzechowski L, et al. Outcome Trends after US Military Concussive Traumatic Brain Injury. J Neurotrauma. 2017;34(14):2206-2219. doi:10.1089/neu.2016.443
- O’Neil ME, Carlson K, Storzbach D, Brenner L, Freeman M, Quiñones A, Motu’apuaka M, Ensley M, Kansagara D. Complications of Mild Traumatic Brain Injury in Veterans and Military Personnel: A Systematic Review [Internet]. Washington (DC): Department of Veterans Affairs (US); 2013 Jan. PMID: 24600749.
- Silver, J.M., T.W. McAllister, and D.B. Arciniegas. Textbook of Traumatic Brain Injury. American Psychiatric Publishing, 2018. https://books.google.com/books?id=ViKMDwAAQBAJ.
- Hadanny A, Abbott S, Suzin G, et al. Effect of hyperbaric oxygen therapy on chronic neurocognitive deficits of post-traumatic brain injury patients: retrospective analysis. BMJ Open 2018;8:e023387. doi: 10.1136/bmjopen-2018-023387 https://bmjopen.bmj.com/content/bmjopen/8/9/e023387.full.pdf
- Boussi-Gross R, Golan H, Fishlev G, et al. Hyperbaric oxygen therapy can improve post concussion syndrome years after mild traumatic brain injury – randomized prospective trial. PLoS One 2013;8(11):e79995 https://www.ncbi.nlm.nih.gov/pubmed/24260334
- Efrati S, Ben-Jacob E. Reflections on the neurotherapeutic effects of hyperbaric oxygen. Expert Rev Neurother 2014;14:233–6. https://www.tandfonline.com/doi/full/10.1586/14737175.2014.884928
- Munivenkatappa, Ashok, et al. “EEG Neurofeedback Therapy: Can It Attenuate Brain Changes in TBI?” NeuroRehabilitation, vol. 35, no. 3, IOS Press, Jan. 2014, pp. 481–84. content.iospress.com, doi:10.3233/NRE-141140.
- Bennett, Cathlyn N., et al. “Clinical and Biochemical Outcomes Following EEG Neurofeedback Training in Traumatic Brain Injury in the Context of Spontaneous Recovery:” Clinical EEG and Neuroscience, SAGE PublicationsSage CA: Los Angeles, CA, Dec. 2017. Sage CA: Los Angeles, CA, journals.sagepub.com, doi:10.1177/1550059417744899.
- Reddy, Rajakumari Pampa, et al. “Silent Epidemic: The Effects of Neurofeedback on Quality-of-Life.” Indian Journal of Psychological Medicine, vol. 36, no. 1, 2014, pp. 40–44. PubMed Central, doi:10.4103/0253-7176.127246.
- Reddy, Rajakumari P., et al. “Neurofeedback Training to Enhance Learning and Memory in Patient with Traumatic Brain Injury: A Single Case Study.” The Indian Journal of Neurotrauma, vol. 6, no. 1, June 2009, pp. 87–90. ScienceDirect, doi:10.1016/S0973-0508(09)80037-3.
- Cheng, G., Kong, R.‐h., Zhang, L.‐m. and Zhang, J.‐n. (2012), Mitochondria in traumatic brain injury and mitochondrial‐targeted multipotential therapeutic strategies. British Journal of Pharmacology, 167: 699-719. doi:10.1111/j.1476-5381.2012.02025.x
- KC, Sagan et al. “Vitamin C enters mitochondria via facilitative glucose transporter 1 (Glut1) and confers mitochondrial protection against oxidative injury.” FASEB journal : official publication of the Federation of American Societies for Experimental Biology vol. 19,12 (2005): 1657-67. doi:10.1096/fj.05-4107com
- Zhang, Xiao-Ying et al. “Vitamin C alleviates LPS-induced cognitive impairment in mice by suppressing neuroinflammation and oxidative stress.” International immunopharmacology vol. 65 (2018): 438-447. doi:10.1016/j.intimp.2018.10.020
- https://www.imin-org.eu/images/science/Haug-Report-Bemer_2016_Englisch.pdf
- NIMH » Post-Traumatic Stress Disorder (PTSD). https://www.nimh.nih.gov/health/statistics/post-traumatic-stress-disorder-ptsd#part_155467. Accessed 2 June 2021.
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th edn. American Psychiatric Publishing, Arlington, VA, 2013.
- Michopoulos, Vasiliki, et al. “Posttraumatic Stress Disorder: A Metabolic Disorder in Disguise?” Experimental Neurology, vol. 284, no. Pt B, Oct. 2016, pp. 220–29. PubMed, doi:10.1016/j.expneurol.2016.05.038.
- Mellon, Synthia H., et al. “Metabolism, Metabolomics, and Inflammation in Posttraumatic Stress Disorder.” Biological Psychiatry, vol. 83, no. 10, May 2018, pp. 866–75. PubMed, doi:10.1016/j.biopsych.2018.02.007.
- Edmondson, Donald, et al. “Posttraumatic Stress Disorder and Risk for Coronary Heart Disease: A Meta-Analytic Review.” American Heart Journal, vol. 166, no. 5, Nov. 2013, pp. 806–14. PubMed, doi:10.1016/j.ahj.2013.07.031.
- O’Donovan, Aoife, et al. “Elevated Risk for Autoimmune Disorders in Iraq and Afghanistan Veterans with Posttraumatic Stress Disorder.” Biological Psychiatry, vol. 77, no. 4, Feb. 2015, pp. 365–74. PubMed, doi:10.1016/j.biopsych.2014.06.015.
- Song, Huan, et al. “Association of Stress-Related Disorders With Subsequent Autoimmune Disease.” JAMA, vol. 319, no. 23, June 2018, pp. 2388–400. PubMed, doi:10.1001/jama.2018.7028.
- Miller, Mark W et al. “Oxidative Stress, Inflammation, and Neuroprogression in Chronic PTSD.” Harvard review of psychiatry vol. 26,2 (2018): 57-69. doi:10.1097/HRP.0000000000000167
- Bradley, Rebekah, et al. “A Multidimensional Meta-Analysis of Psychotherapy for PTSD.” The American Journal of Psychiatry, vol. 162, no. 2, Feb. 2005, pp. 214–27. PubMed, doi:10.1176/appi.ajp.162.2.214.
- Jonas, Daniel E., et al. Psychological and Pharmacological Treatments for Adults With Posttraumatic Stress Disorder (PTSD). Agency for Healthcare Research and Quality (US), 2013. PubMed, http://www.ncbi.nlm.nih.gov/books/NBK137702/.
- Passos, Ives Cavalcante et al. “Inflammatory markers in post-traumatic stress disorder: a systematic review, meta-analysis, and meta-regression.” The lancet. Psychiatry vol. 2,11 (2015): 1002-12. doi:10.1016/S2215-0366(15)00309-0
- Miller, Mark W et al. “Oxidative Stress, Inflammation, and Neuroprogression in Chronic PTSD.” Harvard review of psychiatry vol. 26,2 (2018): 57-69. doi:10.1097/HRP.0000000000000167
- Neigh, Gretchen N, and Fariya F Ali. “Co-morbidity of PTSD and immune system dysfunction: opportunities for treatment.” Current opinion in pharmacology vol. 29 (2016): 104-10. doi:10.1016/j.coph.2016.07.011
- Godman, Cassandra A et al. “Hyperbaric oxygen treatment induces antioxidant gene expression.” Annals of the New York Academy of Sciences vol. 1197 (2010): 178-83. doi:10.1111/j.1749-6632.2009.05393.x
- Szeszko, Philip R., and Rachel Yehuda. “Magnetic Resonance Imaging Predictors of Psychotherapy Treatment Response in Post-Traumatic Stress Disorder: A Role for the Salience Network.” Psychiatry Research, vol. 277, July 2019, pp. 52–57. ScienceDirect, doi:10.1016/j.psychres.2019.02.005.
- Akiki, Teddy J., et al. “Default Mode Network Abnormalities in Posttraumatic Stress Disorder: A Novel Network-Restricted Topology Approach.” NeuroImage, vol. 176, Aug. 2018, pp. 489–98. ScienceDirect, doi:10.1016/j.neuroimage.2018.05.005.
- Ros, Tomas, et al. “Mind over Chatter: Plastic up-Regulation of the FMRI Salience Network Directly after EEG Neurofeedback.” NeuroImage, vol. 65, Jan. 2013, pp. 324–35. ScienceDirect, doi:10.1016/j.neuroimage.2012.09.046.
- Kluetsch, R. C., et al. “Plastic Modulation of PTSD Resting-State Networks and Subjective Wellbeing by EEG Neurofeedback.” Acta Psychiatrica Scandinavica, vol. 130, no. 2, 2014, pp. 123–36. Wiley Online Library, doi:https://doi.org/10.1111/acps.12229.
- Kolk, Bessel A. van der, et al. “A Randomized Controlled Study of Neurofeedback for Chronic PTSD.” PLOS ONE, vol. 11, no. 12, Public Library of Science, Dec. 2016, p. e0166752. PLoS Journals, doi:10.1371/journal.pone.0166752.
- Nicholson, Andrew A., et al. “Intrinsic Connectivity Network Dynamics in PTSD during Amygdala Downregulation Using Real-Time FMRI Neurofeedback: A Preliminary Analysis.” Human Brain Mapping, vol. 39, no. 11, 2018, pp. 4258–75. Wiley Online Library, doi:10.1002/hbm.24244.
- Rogel, Ainat, et al. “The Impact of Neurofeedback Training on Children with Developmental Trauma: A Randomized Controlled Study.” Psychological Trauma: Theory, Research, Practice, and Policy, vol. 12, no. 8, Educational Publishing Foundation, 2020, pp. 918–29. APA PsycNET, doi:10.1037/tra0000648.
- Gapen, Mark, et al. “A Pilot Study of Neurofeedback for Chronic PTSD.” Applied Psychophysiology and Biofeedback, vol. 41, no. 3, Sept. 2016, pp. 251–61. Springer Link, doi:10.1007/s10484-015-9326-5.
- Miller, Mark W et al. “Oxidative Stress, Inflammation, and Neuroprogression in Chronic PTSD.” Harvard review of psychiatry vol. 26,2 (2018): 57-69. doi:10.1097/HRP.0000000000000167
- S. Brody, R. Preut, K. Schommer, T.H. Schürmeyer A randomized controlled trial of high dose ascorbic acid for reduction of blood pressure, cortisol, and subjective responses to psychological stress Psychopharmacology (Berl), 159 (2002), pp. 319-324, 10.1007/s00213-001-0929-6
- Peters, E M et al. “Vitamin C supplementation attenuates the increases in circulating cortisol, adrenaline and anti-inflammatory polypeptides following ultramarathon running.” International journal of sports medicine vol. 22,7 (2001): 537-43. doi:10.1055/s-2001-17610
- Michels L, Schulte-Vels T, Schick M, O’Gorman RL, Zeffiro T, Hasler G, et al. Prefrontal GABA and glutathione imbalance in posttraumatic stress disorder: preliminary findings. Psychiatry Res. 2014;224(3):288–95.
- Ross, Christina L., et al. “The Use of Pulsed Electromagnetic Field to Modulate Inflammation and Improve Tissue Regeneration: A Review.” Bioelectricity, vol. 1, no. 4, Mary Ann Liebert, Inc., publishers, Dec. 2019, pp. 247–59. liebertpub.com (Atypon), doi:10.1089/bioe.2019.0026.



