The Riemenschneiders were reeling over their toddler’s bloodied face and lacerated lip when they received another shock in the Children’s Minnesota emergency room in St. Paul.
Two-year-old Kenzie had lost the top third of her ear from a severe dog bite, and a doctor wanted to try an ambitious hyperbaric oxygen therapy to save it.
“We were just adrenaline-driven at that point. I didn’t want anything to do with any decisions,” said the mother, Jaisa Riemenschneider, who recalled thinking, “Let’s just trust the doctor and let’s get going.”
The quick decision proved smart. Surgery reattached the ear fragment after the Nov. 2 injury, and then 40 days of hyperbaric treatments at Hennepin Healthcare in Minneapolis helped it grow healthy blood vessels and return to life.
“Seeing her ear turn gray, then black, and then slowly starting to see skin color come back?” her mother said. “You just never thought that a body part could change colors like that.”
Doctors from both institutions are writing an academic paper to teach others about this promising expansion of hyperbaric medicine — a specialty that increases the lungs’ distribution of oxygen to tissues by placing patients inside sealed, high-air-pressure chambers.
Surgery alone had little chance of success, but Children’s Dr. Siva Chinnadurai believed hyperbaric therapy could improve the odds enough to try it on Kenzie. A similar approach a few weeks earlier had been successful in treating a 10-year-old’s wound but, as far as Chinnadurai knew, that was the world’s first attempt at combining an ear reattachment procedure with hyperbaric treatment.
It wasn’t the only fortunate decision. Kenzie’s bloodied face made it difficult to identify the ear wound when paramedics arrived at the family’s home in Houlton, Wis. As they were preparing for the trip to the hospital, one paramedic noticed an ear fragment that fell out of the girl’s sweater and put it on ice.
‘Clock starts ticking’
The general rule is that tissue or skin grafts need to happen within 72 hours to work, but that timeline probably shrinks when dealing with ears, Chinnadurai said.
“You immediately start having cell death right away when the blood supply is interrupted,” he said. “So that clock starts ticking almost right away.”
Hyperbaric chambers in oceanside hospitals often treat decompression sickness in divers who surface too quickly. HCMC’s unit often treats adults with burn injuries, frostbite, wounds and carbon monoxide poisoning — though one memorable case involved a diver who ascended too quickly from a shipwreck in Lake Superior and spent 53 straight hours in a chamber.
Children, much less toddlers, aren’t common patients in the unit.
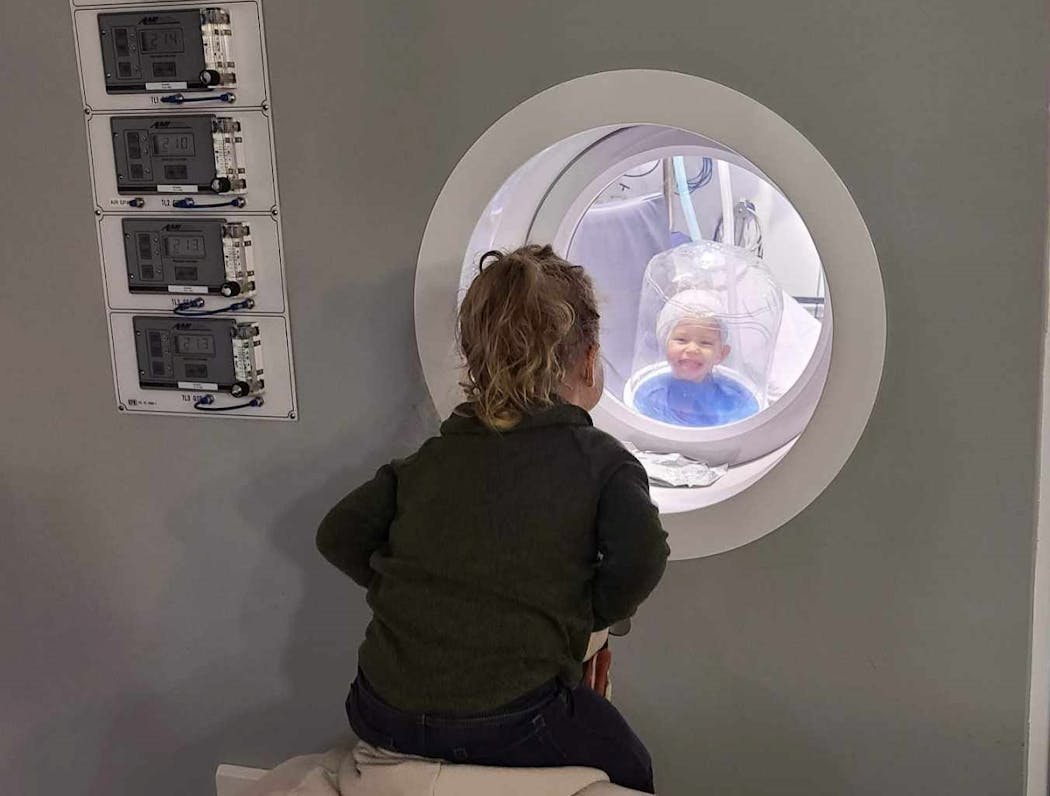
“We didn’t know exactly what it was. We were like, ‘Yeah, right. You’re going to stick her in a tube? Good luck,'” said her father, Andy Riemenschneider. “We didn’t know it was a whole room like this.”
Stress from the ordeal probably didn’t help, she said: “I still had blood in my hair. I hadn’t been home yet.”
A happy patient
After that, Kenzie received treatments with nurses or technicians in the chamber. Her bravery and bubbly nature won over the entire unit. Several caregivers returned off-duty on Tuesday to see her during a return visit.
“She was a dream in the chamber — bonded with all of our nurses,” said Dr. Tom Masters, the hyperbaric medicine specialist who oversaw Kenzie’s treatment. “She did really well. We were concerned about it, but it turned out to be something she could handle.”
Kenzie is happy back home with her parents and 3-year-old sister, showing few if any signs of mental anguish from the attack or the prolonged treatment.
The puppy that bit Kenzie has been adopted by another family. It was a brief, freak incident that might have occurred when Kenzie accidentally yanked the excited puppy’s collar, her father said. The family still has cats and another puppy. Kenzie plays with the dog — sometimes cautiously.
“She still loves animals,” her father said.
Cited by STAR TRIBUNE