Concussions are a type of traumatic brain injury (TBI) caused by a blow or jolt to the head or body, resulting in the brain rapidly moving back and forth inside the skull. While they are often considered mild injuries, concussions can have serious and lasting effects...
Brain Damage
Hyperbaric Oxygen Therapy (HBOT) Research for Brain Damage.
Doctors at Sakra World Hospital does miraculous Neuro-rehabilitation of 36-year-old with severe head injury following bike accident in US
Hyperbaric Oxygen Therapy helps heal a severe traumatic brain injury in India! Not all hopes die if you know the way out and believe in miracles. When 36-year-old Mr. Pravin Raj Radha met with a fatal accident in the US after he fell from his bicycle in May 2022, he...
Hyperbaric oxygen therapy in children with post-concussion syndrome improves cognitive and behavioral function: a randomized controlled trial
Abstract Persistent post-concussion syndrome (PPCS) is a common and significant morbidity among children following traumatic brain injury (TBI) and the evidence for effective PPCS treatments remains limited. Recent studies have shown the beneficial effects of...
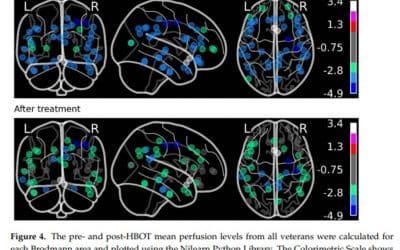
A Case Series of 39 United States Veterans with Mild Traumatic Brain Injury Treated with Hyperbaric Oxygen Therapy
Abstract: Importance: The Defense and Veterans Brain Injury Center reported 358,088 mild traumatic brain injury (mTBI) among U.S. service members worldwide between the years 2000 and 2020. Veterans with mTBI have higher rates of Post-Traumatic Stress Disorder (PTSD),...
MORE IS BETTER: THE RECURRENT ILLUSION OF HIGHER PRESSURE HBOT IN CHRONIC BRAIN INJURY PAUL G. HARCH, M.D.
Image Credits: Harch HBOTIn the past two years a disturbing trend has become a standard of care in the off-label use of HBOT for chronic pediatric brain injury, the use of 1.75 ATA oxygen. Unfortunately, this is merely the latest re-emergence of the age old illusion...
Can Hyperbaric Oxygen Heal Your Brain?
Research supports hyperbaric oxygen therapy as a treatment for mild brain injuries and Alzheimers disease, but it remains controversial as a treatment for autism.(Nakleyka/Shuttertock) A new study shows promising results for this alternative treatment BY JENNIFER...
Systematic Review and Dosage Analysis: Hyperbaric Oxygen Therapy Efficacy in Mild Traumatic Brain Injury Persistent Postconcussion Syndrome
Background: Mild traumatic brain injury results in over 15% of patients progressing to Persistent Postconcussion Syndrome, a condition with significant consequences and limited treatment options. Hyperbaric oxygen therapy has been applied to Persistent Postconcussion...
Changes in attentional processing following neurofeedback in patients with persistent post-concussive symptoms: a pilot study
Abstract Objective: Persistent post-concussive symptoms (PPCS) often include attention deficits, particularly orienting and executive attention. Research in other clinical populations has demonstrated that neurofeedback therapy (NFT) is effective at improving...
Systemic Inflammation Persists the First Year after Mild Traumatic Brain Injury: Results from the Prospective Trondheim Mild Traumatic Brain Injury Study
Abstract Innate immune activation has been attributed a key role in traumatic brain injury (TBI) and successive morbidity. In mild TBI (mTBI), however, the extent and persistence of innate immune activation are unknown. We determined plasma cytokine level changes over...