Treat Brain Wounds with Hyperbaric Oxygenation and other Alternative Therapies "VA’s top clinical priority is preventing suicide among all Veterans — including those who do not, and may never, seek care within the VA health care system.” Yet nowhere in their...
Post-Traumatic Stress Disorder (PTSD)
Hyperbaric Oxygen Therapy (HBOT) Research for Post-Traumatic Stress Disorder (PTSD)
A Case Series of 39 United States Veterans with Mild Traumatic Brain Injury Treated with Hyperbaric Oxygen Therapy
Abstract: Importance: The Defense and Veterans Brain Injury Center reported 358,088 mild traumatic brain injury (mTBI) among U.S. service members worldwide between the years 2000 and 2020. Veterans with mTBI have higher rates of Post-Traumatic Stress Disorder (PTSD),...
Israeli study: oxygen therapy working for PTSD
OXYGEN therapy can dramatically reduce post-traumatic stress disorder, according to a world-first Israeli study on Israel Defense Force veterans, during which half the subjects made such good progress they were no longer deemed to have PTSD. The Tel Aviv...
Israeli Study of IDF veterans shows oxygen therapy reduces PTSD symptoms
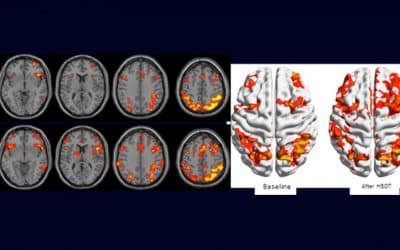
Clinical example of functional brain imaging by fMRI. The reduced brain activity in the frontal lobes of the brain and in hippocampus is improved after Hyperbaric Oxygen Therapy . Credit: Shamir Medical Center Israeli scientists have found that...
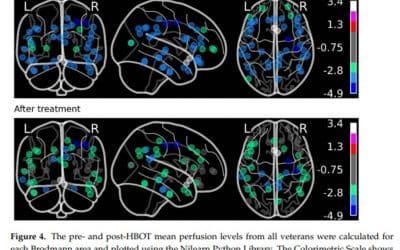
Hyperbaric oxygen therapy improves symptoms, brain’s microstructure and functionality in veterans with treatment resistant post-traumatic stress disorder: A prospective, randomized, controlled trial
Abstract Introduction Post-traumatic stress disorder (PTSD) is characterized by changes in both brain activity and microstructural integrity. Cumulative evidence demonstrates that hyperbaric oxygen therapy (HBOT) induces neuroplasticity and case-series studies...
Hyperbaric oxygen therapy for mild traumatic brain injury persistent postconcussion syndrome: a randomized controlled trial
Abstract: Persistent postconcussion syndrome (PPCS) after mild traumatic brain injury (mTBI) is a significant public health and military problem for which there is limited treatment evidence. The aim of this study was to determine whether forty 150 kPa hyperbaric...
Retrospective Case Series of Traumatic Brain Injury and Post-Traumatic Stress Disorder Treated with Hyperbaric Oxygen Therapy
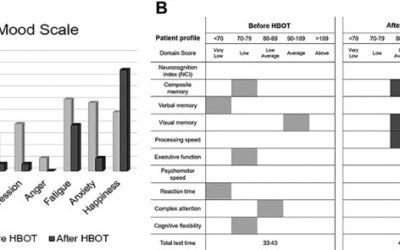
Returning veterans are frequently diagnosed with traumatic brain injury (TBI) and post-traumatic stress disorder (PTSD). Considering a recent case-controlled study of hyperbaric oxygen therapy (HBOT) reporting a reduction in suicidal ideation, we investigated retrospectively three veterans with chronic TBI/PTSD symptoms who were treated with multiple rounds of HBOT with neurophysiological testing performed before and after treatment. Improvements were detected on parameters within neurocognitive domains, including reductions in suicide-related symptoms. These findings independently confirm that HBOT may be effective in treating specific symptoms of TBI/PTSD that are not currently addressed with existing therapeutic approaches.
Evidence brief: hyperbaric oxygen therapy (HBOT) for traumatic brain injury and/or post-traumatic stress disorder.
This report is a product of the VA Evidence-based Synthesis Program. The purpose is to provide “timely and accurate syntheses of targeted healthcare topics. to improve the health and healthcare of Veterans”. The authors have made a comprehensive search and analysis of the literature and make recommendations to assist clinicians in dealing with veterans suffering from either traumatic brain injury (TBI) or post-traumatic stress disorder (PTSD). The report is timely and of great potential impact given the vigorous and lengthy debate among hyperbaric physicians and lay people determined to find an answer for the large numbers of veterans deeply affected with some combination of PTSD and post-concussion dysfunction.
HYPERBARIC OXYGEN THERAPY- BASICS AND NEW APPLICATIONS
Hyperbaric oxygen therapy (HBOT) serves as primary or adjunctive therapy for a diverse range of medical conditions. The indication for HBOT can be related to either pressure (decompression sickness or air emboli) or tissue hypoxia. It is now realized, that the combined action of hyperoxia and hyperbaric pressure, leads to significant improvement in tissue oxygenation while targeting both oxygen and pressure sensitive genes, resulting in improved mitochondrial metabolism with anti-apoptotic and anti-inflammatory effects. Clinical studies published in recent year’s present convincing evidence that HBOT can be the coveted neurotherapeutic method for brain repair. Here we discuss the multi-faceted role of HBOT in wound care in general and in neurotherapeutics in detail.